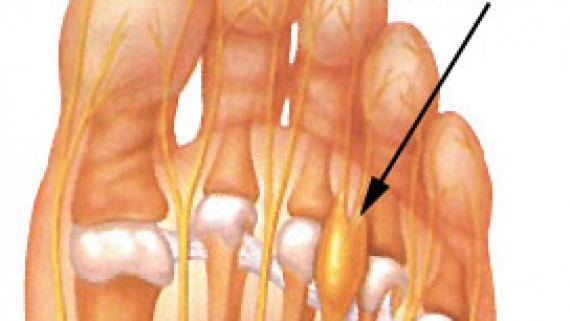
What is a Morton’s neuroma?
How did I get this?
If I had a Morton’s neuroma, what would it feel like?
What do I do next?
- Ice to the area
- Again ladies – avoid high heels!
- Check the width of your footwear. Try wearing wider shoes with a lower heel. Tighter or narrow footwear can compress and bunch the toes together. Your podiatrist can help you with footwear assessment and recommendations.
The exact cause of Morton’s neuroma can be different between patients. An accurate diagnosis can be made by a podiatrist.
- You may require orthotics to alleviate the forefoot pressure and mechanics in combination with metatarsal padding.
- Additional, ultrasound imaging maybe required to consider other diagnostic possibilities (as mentioned in first post).
- In more serve cases a course of anaesthetic and cortisone injections.
- Surgical removal of the neuroma as last resort.
Don’t forget, a neuroma is a result of a nerve that is being traumatised by a poorly functioning foot or footwear and treating the cause of this condition is paramount.
Metatarsalgia – Ball of Foot Pain
So many foot problems can occur in our forefoot. As podiatrists we treat a wide range of problems associated with forefoot pain and deformity. Metatarsalgia is a non-specific term or general umbrella term if you will, for pain in the forefoot or ball of the foot.
Discomfort is usually located beneath the balls of our feet and is typically a result of increased forefoot pressure.
Bunions, hammertoes, short metatarsal bones, stress fractures, plantar plate disruption, Freiberg’s infarction, capsulitis, intermetatarsal bursitis and Morton’s neuroma area some possible causes of metatarsalgia.
Today we are talking about intermetatarsal bursitis.
Intermetatarsal bursitis
What is bursitis?
An inflammation or irritation of the bursa. A bursa is a small fluid-filled sac that provides cushioning and reduces friction, between and around the joints of the forefoot. Irritation of the bursa can cause swelling and pain (bursitis). The intermetatarsal bursae are located on the bottom of the foot near the base of the toes.
Bursitis can also affect other parts of the body – back of the heel/Achilles tendon, the knee, hip, shoulder and elbow.
How did I get this?
Generally, bursitis can occur through injury or repetitive motion causing irritation and inflammation. They can become irritated when one metatarsal bone takes more load than others.
Wearing narrow or excessively worn footwear during the day and different sporting activities can increase your chance of developing bursitis. Other factors can include;
- Overuse or excessive pressure on the forefoot
- Stress from abnormal foot mechanics
- Injury from a fall or hit to the area
- Less commonly due to certain types of arthritis; rheumatoid arthritis, gout, psoriatic arthritis
If I had bursitis, what would it feel like?
Friction can cause the space between the tendon, bone and skin to become inflamed – causing swelling, pain and possibly redness of the surrounding area.
Irritation and restricted movement of the affected joint may be evident and certain footwear or activities may exacerbate pain.
What do I do next?
- Apply ice to the area – this can help reduce inflammation
- Rest and avoid painful activities
- Non-steroidal anti-inflammatories if advised by your pharmacist
- Orthotics
- Footwear changes, avoid high heels!
- Reduce the amount of pressure being place placed on the bursa through off loading
- In chronic cases, injections of local anaesthetic and corticosteroid may be required in combination with padding
It’s important to attend a podiatry consult for assessment to determine the root cause, as other injuries can produce similar symptoms. Podiatrist may advise you on appropriate shoes and can also add padding to off load the pressure, prescribe orthotics and refer for any imaging that may be needed to rule out other conditions.
Contact us on 1300 847 226 or make an appointment online to speak with one of our friendly podiatrists about helping you get back on your feet sooner!
The battle of the fungal nail!
Fungal toenails or onychomycosis is common, unpleasant and persistent in nature. Accounting for almost half of all nail problems, this slow growing infection occurs when microscopic fungi gain entry to the nail, usually through small trauma. Trauma allows the pathogen to enter the nail and nail bed.
Other causes
- Fungal organisms grow and spread in warm, moist environments and are usually picked up in warm damp areas like socks, shoes, public pools, gyms and showers.
- Not drying off the feet thoroughly following showers or exercise and wearing tight shoes or socks, can provide conditions the fungus needs for growth.
- People who have a compromised immune system, diabetes, circulatory problems and the elderly are particularly susceptible.
Symptoms
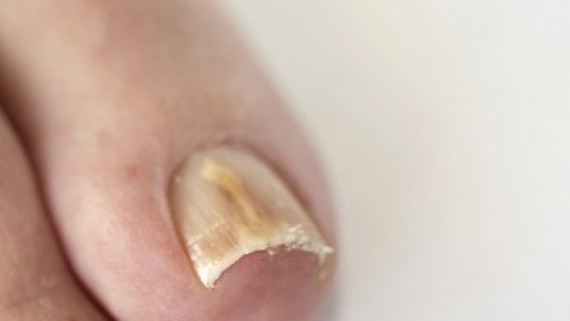
Fungal nail infections are contagious and can often spread from skin to nails. The poor cosmetic appearance that usually develops can cause some embarrassment. Nails can become discoloured, thickened, brittle, rough and weaken. Sometimes the infection can occur with an odour and can cause discomfort.
Types of Onychomycosis
Distal subungual onychomycosis – most common form of fungal nail that can cause the nail to become yellow brownish in colour, thickened, rough or crumbling.
Superficial white onychomycosis – this type of infection occurs on the outer surface and often appears as white spots. It is the easiest type of infection to treat.
Proximal subungual onychomycosis – occurs in the area of new nail growth at the beginning of the nail and is the least common.
Candida onychomycosis – typically occurs after trauma or damage to the nail that allows the fungus to invade. Most often occurs in people who frequently have their feet in water.
Treatment
As many people with fungal toenails can appreciate, it’s often difficult to eradicate fungal toenail infections, and like most things, prevention is always better than cure. Treatment varies depending on the type of fungal nail infection and the amount of nail involved, so it’s best to chat to your podiatrist who can recommend the best treatment option for your type of onychomycosis. In many cases nail lacquer medications are used, and in severe cases oral antifungal medication from your doctor, however this comes with potential side-effects.
Preventative measures
- Wear protective shoes in public showers and pool areas.
- Wash your feet regularly and dry them thoroughly when they get wet.
- Change socks daily, more regularly if you have increase perspiration or exercise.
- Avoid leaving toenail polish in place for long periods of time, wearing nail polish is not advised for those people who are suffering from nail fungus as it may encourage it to grow.
- Avoid nail solons who re-use their nail instruments, all instruments should be sterilised using an autoclave.
- Wear properly fitting shoes
If you suspect a toenail fungus, it’s recommended you see your podiatrist before it spreads. Podiatrists also have a tool to reduce thickness of fungal nails, this can enable topical medication to absorb and penetrate the nail easier, provide comfort of thickened nails and can help improve the appearance of the nail.
If you or someone you know would benefit from fungal nail treatment, please give us a call or book an appointment online at any of our podiatry clinics in Warragul, Drouin, Beaconsfield or Cranbourne.
Understanding the need to look after your feet when you have diabetes
What is diabetes?
The pancreas is no longer able to make insulin, or the body cannot make good use of the insulin it does produce.
Insulin enables glucose (sugar), from the food we eat to pass from the blood stream into the cells in the body to make energy.
Not being able to produce insulin or use it effectively can cause raised sugar levels (hyperglycaemia). Over the long-term high sugar levels can damage some tissues and organs in the body.
Type 1 diabetes is usually caused by an auto-immune reaction where the body’s defence system attacks cells that produce insulin. It can occur at any age, however it is more common in children or young adults. Injections of insulin to control sugar levels in the blood is required.
Type 2 diabetes occurs when the body is no longer using insulin efficiently. Sugar builds up in bloodstream and the cells are starved of energy. There may be a family history to developing type 2 diabetes or environmental triggers.
Diabetes and the feet come hand in hand (or foot in foot).
“Every year, more than 4,400 amputations are carried out as a result of diabetes”. (https://www.diabetesaustralia.com.au/national-diabetes-week). Foot complications with diabetes are becoming more prevalent. Prevention through education, understanding foot complications, signs and symptoms and regular assessment is required to prevent hospitalisation and risk of amputation.
Some foot concerns:
- Nerve damage (peripheral neuropathy) and poor circulation in the feet (peripheral arterial disease).
- Loss of feeling, tingling, burning sensation and numbness.
- Poor healing, cramping.
- Increase rate of infection.
- Foot ulcers or sores that may have delayed healing.
- Changes in shape which can cause an increase in pressure .
- Hammer or claw toes, bunions, arthritis.
- Charcot’s arthropathy.
- A rare condition that occurs with good blood flow to the feet and numbness (peripheral neuropathy) – red, hot, swollen foot, rocker bottom foot.
Peripheral neuropathy explained
- Insensitivity or loss of ability to feel; touch, pressure, vibration, pain, heat, cold or perception/position.
- You may not realise you have a cut, blister, corn or footwear rubbing. The damage caused may not heal adequately, which may cause ulceration in some cases.
- Check feet daily for cuts and redness and blisters etc.
Poor circulation explained
- Reduced blood flow and nutrients to the feet
- Swelling and dryness and impaired healing process
- Cold feet
- Painful calves when walking or at night in bed
- Delayed or reduced healing rate in the feet
- Improve – activity, avoid smoking, reduce caffeine
- Control cholesterol and blood sugar levels
Regular podiatry and foot check-ups or assessments are an important part of preventative care for your feet to prevent serious complications. Diabetes assessment every 3-12 months and more regularly treatment for hard skin, corns and nail care is recommended.
Quick and painless tests by your podiatrist include:
- Vascular assessment with an ultrasound testing the amount of blood flow to the feet.
- Neurological assessment testing sensation and your ability to feel.
- Gait (Walking) assessment to assess any increase in pressure due to the change in foot shape.
- Footwear assessment to ensure suitable footwear and fit.
- Skin and nail care to prevent any ingrowing toenails, painful corns and pressure areas.
Preventing foot complications and self-managing tips
- Control your blood sugar levels to reduce the risk of damage to your feet.
- Keeping moving! Blood flow is important for healthy feet.
- Stop smoking – smoking slows down blood flow to the extremities.
- Check feet daily – with a mirror to observe for any cuts or red marks that require attention.
- Good foot hygiene is important. Wash and dry your feet thoroughly daily.
- Be careful with trimming toes nails and avoid cutting down the side.
- Wear comfortable socks and shoes.
- Get fitted professionally for shoes at the end of the day to reduce risk of poorly fitting shoes causing blisters.
- Avoid uncomfortable or tight shoes that rub or cut into your feet.
- Avoid high heels and pointed toes.
- Look inside your shoes daily for any stones, or prominent lining to avoid rubbing against your feet causing blisters.
- Avoid walking barefoot.
- Wear comfortable socks that are a good fit and aren’t too tight.
- Prevent dry skin by applying moisturise daily, avoid cream between the toes.
- See a podiatrist regularly to trim off callous, remove corns and trim toenails.
- Podiatry diabetes assessment.
In summary…
Of course not all foot problems will require a hospital visit, but they can vary from minor complications to wounds that won’t heal. Serious complications can be avoided through self-management and through regular check-ups.
Simple injuries such as corns, cuts, or callouses, when combined with loss of sensation in the feet can mean that these injuries go unnoticed. If untreated they may not heal due to lack of blood supply and infection can occur. Foot assessment by a podiatrist is recommended to establish your foot health status by determining the blood flow and sensation in your feet and identify any potential risk areas.
- Look at your feet daily.